I realize that this is a controversial subject and that many have opinions on it. I have my own opinions; having used cannabis during all of my pregnancies. And while I would not advocate usage of cannabis during pregnancy to anyone (this is a personal decision for everyone), I know how it helped me through the nausea and discomforts... and also afterwards with postpartum depression. Both of my children were born healthy and with high IQ's.... so there was no damage done by using cannabis during the pregnancies.
CANNABIS USE DURING PREGNANCY: IS IT SAFE?
Dr. Stacey Kerr discusses the controversial topic of cannabis use during pregnancy and gives highlights from her clinical experience with expecting mothers.
Pamela is newly pregnant with her third child. She and her husband think this is going to be their last one because she is having a dreadful time with nausea – morning sickness that lasts all day long. She knows all the tricks. Saltines by her bedside, taking Vitamin B6 and B12, and eating frequently even though her stomach is queasy. She tried ginger. She tried acupuncture. She considered hypnosis. None of it is working, and the added stress of two little ones who still need her attention is making her pregnancy a miserable experience. She really wants this baby, but lately she’s been having guilty doubts about whether it’s worth going through all the nausea and vomiting.
Pamela consulted her physician. She was offered some prescription medications – droperidol (an antipsychotic), metoclopramide (causes drowsiness & dizziness), Benedryl (drowsiness), or Zofran. Although her doctor reassured her about side effects and effects on her baby, she really did not want to take a pharmaceutical if she could avoid it.
Pamela had used cannabis occasionally for many years. It relieved her stress at the end of the day when the kids were finally in bed and she had time to herself. It helped ease some pain she had in the past, and aided sleep when she had short bouts of insomnia. She knew it could help with nausea, appetite, and stress, but she did not know if it was safe to use it while pregnant. So she searched online for facts.
Online, Pamela found conflicting information. Some sites said it was perfectly fine to use cannabis while pregnant. Others warned of brain damage, early labors, babies with failure to thrive, and other dire consequences. There seemed to be some research on the subject, but was it well done? Was it reliable? How was she to dig down and find the real story?
USING CANNABIS WHILE PREGNANT
I am a family physician and have attended hundreds of births during my career. I live in an area of the country (Northern California) where cannabis is used by many of my patients, and when they discovered that they could be honest with me about their use my prenatal records became more complete.
Many mothers use cannabis for nausea and for stress relief.
Many mothers were using it for nausea and for stress relief. Some used it because it was simply part of their lifestyle. We discussed this during their visits, and I was clear with them that I honestly did not know if cannabis caused harm because the scientific research was still incomplete.
In my experience, however, I had not seen complications from cannabis – but I had seen complications from alcohol and other drugs. We discussed the difference between ‘use’ and ‘abuse.’ If they planned to use it I, encouraged conscious use; microdosing to treat the need without overusing.
However, my personal and professional experience was not enough to rely on as a source of information for my patients. I began a search and review of the literature, reading the published peer-reviewed articles, and evaluating the study designs and the outcomes.
FACTS AND RISKS
In this article, we are going to look at the facts. We will look at the research and outcomes, and evaluate their worth. We will look at populations that used cannabis during pregnancy and see how their children are doing now. The information shared may help you make your own decision about using cannabis during pregnancy.
It is important to remember that pregnancy recommendations regarding what to eat, what to drink, what medications to take, and any other outside influences are fraught with caution and fear. If the child does not turn out ‘right,’ who’s fault is it? Pointing a finger of blame can lead to guilt, to lawsuits, and/or a lifetime of regret. Simply being pregnant and carrying a baby for nine months creates unavoidable risks for both mother and baby. But for some, there is no end to the perceived risks or possible harms a mother may cause an unborn child.
Note: The use patterns considered here are limited to well-considered, clearly needed uses of cannabis.This includes using the herb or its constituents for medical reasons such as nausea, pain, sleep, or possibly for stress relief. I encourage any cannabis use to be done consciously, with respect for its power as medicine.
ENDOCANNABINOIDS ARE ESSENTIAL
Before we look at introducing phytocannabinoids to a pregnant mother, let’s consider the endocannabinoid system and the critical role it plays in creating new life. It turns out that our own endocannabinoids, those we create ourselves, are essential to fertilization, growth of the fetus, and survival of a newborn.
LOW BIRTH WEIGHT, PRETERM LABOR, INCREASED NICU ADMISSIONS?
With the use of cannabis we worry about miswiring the baby’s brain, causing an increase in pregnancy and delivery complications, admissions to the intensive care unit, and problems later in the child’s life such as psychiatric conditions, poor academic achievement, and increased addiction disorders. The possibility of harm caused by using cannabis is a fearful possibility to many pregnant women, their physicians, and midwives.
The most often quoted article in my community was work published in 2011 by Hayatbakhsh and his team, covering a 7-year span of observation in Australia. They interviewed almost 25,000 pregnant women, with over 2400 of these women admitting to ever using cannabis and 637 admitting to use at the time of the interview, during their pregnancy. His conclusions were:
“Use of cannabis during pregnancy strongly and significantly predicted negative birth outcomes, including low birth weight (375 g/.8 lbs lighter), preterm birth, small size for gestational age, and increased admission to the NICU (neonatal intensive care unit).”
Because I had not seen this trend in my own community I read his research carefully. They had controlled for socioeconomic status, multi-substance use, and took into consideration the use of alcohol, cigarettes, and other illicit substances. Their results remained statistically significant.
“Research has suggested that between 8-29% of women use cannabis during pregnancy.”
I kept looking until I found the problem with Hayatbakhsh’s data. First, it was with the method of collection. Pregnant women were interviewed as part of a routine second trimester interview at a public, not private, maternity hospital. Midwives entered the data into a computer, and anyone admitting current use was offered directed care through the hospital’s alcohol and drug specialist service. Any admitted past use was followed by questions on current use.
Now imagine yourself sitting across a desk from a midwife who is providing your care while you are in a vulnerable, pregnant state. She asks you about drug use. Do you tell the truth? Do you admit to something that triggers a referral to a special service for drug abusers? If you answered “yes” to this, you are in the minority. A self-selected group such as this will not lead to the best data, with evidence skewed depending on how many young women were able to be truthful about their use of cannabis.
Surveys done elsewhere support my concern in the data collection process. “Seven percent of pregnant women self-report using marijuana during the prior 2–12 months, although studies measuring marijuana use by self-report or urine screens have identified prevalence ranging from 8% to 29% .”
In addition, there was no long-term follow-up done on any of the mothers or babies from the positive cohort. These weaknesses in the study were enough for me to consider the data questionable. I moved on to the next concern.
ABNORMAL NEURODEVELOPMENT?
Miswiring the brain is a drastic, dramatic, scary thought. No one wants to think they have any avoidable part in harming a baby’s brain. This is a truly serious concern.
A study published in 2011 showed that THC disrupts the natural, highly efficient endocannabinoid signaling in the fetal brain. CB1 receptors in the brain are integral to the development of neural pathways in the developing fetus. The study found that if present, THC will bind to these receptors rather than endocannabinoids.
Researchers dissected brains that tested positive for THC and found those brains to have less of a naturally occurring protein called SCG10, a protein that regulates neuron development. The authors hypothesized that this decrease in SCG10 could cause neurons to develop abnormally both in structure and direction.
Based on an observation, researchers proposed one hypothesis. An alternate hypothesis could be that THCis as efficient as the endocannabinoids. A third hypothesis could be that THC is even more efficient than SCG10. We simply do not know. From this study, all we know is that THC does “promiscuously bind to members of the cannabinoid receptor family.”
Children exposed to marijuana, and not alcohol, in utero were almost 50% better at a behavioral measure of brain processing than controls.
There is an accepted way to measure abnormal neurodevelopment that has been used to evaluate problems like dyslexia, autistic spectrum disorder, and fetal alcohol syndrome. Global Motion Perception (GMP) is a behavioral measure of a type of brain processing that is thought to be particularly vulnerable to abnormal neurodevelopment. GMP is the ability to perceive the whole, rather than focusing only on the individual parts. Imagine watching a football half-time show and being unable to appreciate the pattern the band makes across the field, forced to see only a single tuba player. Those with impaired GMP would only be able to see that tuba player, unable to appreciate the whole picture.
A study published in 2015 measured GMP in 145 4.5-year-old children who had been exposed to different combinations of methamphetamine, alcohol, nicotine, and marijuana prior to birth along with 25 unexposed children. The results were surprising.
As expected, GMP was impaired by prenatal exposure to alcohol. But it was improved significantly by exposure to marijuana! And the direction and size of the effect was unexpected; the children exposed to marijuana in the absence of alcohol were almost 50% better at the GMP task than children with no marijuana exposure. Global motion perception for children exposed to both marijuana and alcohol was no different from that of children who had no drug exposure. Only alcohol and marijuana exposure had independent effects on global motion perception after controlling for the effects of multiple drug exposure, verbal IQ, ethnicity, habitual visual acuity, and sex. Alcohol to the negative, marijuana to the positive.
ACADEMIC ACHIEVEMENT?
The information about neurodevelopment was reassuring, so I moved on to my next concern: academic achievement later in the child’s development. Goldschmidt and his team published research in 2011 that concluded, “First trimester exposure to cannabis significantly predicted poorer academic achievement scores at 14 years of age.”
Here was some long-term follow-up that could be significant.
This research was more difficult to evaluate. It looked like they had accounted for all the possible variables: prenatal alcohol use, tobacco, cigarettes, and other illicit drug exposure. Still, I had not seen this effect of cannabis in my own practice after years of delivering babies and watching those children grow up. What could be the difference?
I called a statistician. After his review, he educated me about ‘mediators.’ Mediators are the factors that must come into play to cause the seen effects. In this case, there were four mediators listed here in order of importance:
SEVERE MENTAL ILLNESS?
Moving to the next concern, I wondered about the possibility of increased incidence of severe mental illness in children exposed to cannabis during gestation, especially if there was a history of mental illness in the family. This went along with the theory of miswiring brains; if brains were miswired by THC, would this trigger schizophrenia? If teens used cannabis, would they be more likely to develop schizophrenia?
Harvard University and the Boston VA looked at this possibility. The question they set out to answer: “Is family risk for schizophrenia a crucial factor underlying the association between the development of schizophrenia in teens who smoke marijuana?”
They looked at 282 individuals from the New York and Boston metropolitan areas. They gathered information on 1,168 first-degree relatives and a total of 4,291 relatives. They collected information regarding cannabis use, and family history regarding schizophrenia, bipolar disorder, depression, and drug abuse. What they found was that the tendency for depression and bipolar disorder was dependent on family history of these disorders. Their conclusion: “Having an increased familial risk for schizophrenia is the underlying basis for schizophrenia in these samples — not the cannabis use.”
LARGE STUDIES?
Still not completely reassured or satisfied with the available research, I looked for more, and found a study from Carleton University in Ottawa, Canada. Since 1978, psychologist Peter Fried and his colleagues collected longitudinal data on prenatal marijuana exposure as part of the Ottawa Prenatal Prospective Study (OPPS). These researchers administered hundreds of tests to the same group of about 145 children over a 22-year period. The group assessed physical development, psychomotor ability, emotional and psychological adjustment, cognitive functioning, intellectual capacity, and behavior.
At the end of this extensive, long-term study, they found very few differences between marijuana-exposed and nonexposed children. After controlling for known confounding variables, Fried estimated that prenatal drug exposure to alcohol, tobacco, and marijuana combined accounted for 8 percent or less of the variance in children’s scores on developmental and cognitive tests.
Researchers found very few differences between marijuana-exposed and non-exposed children.
Furthermore, no review of this topic would be complete without looking at the work done by Melanie Dreher, a pediatrician who published in the journal Pediatrics in 1994. She looked at children exposed to cannabis in Jamaica. It was a relatively small study – looking at 24 newborns exposed to marijuana prenatally and 20 nonexposed newborns. She found that there were no significant differences between exposed and nonexposed infants on day 3. Then, at 1 month, she found that the exposed infants showed better physiological stability. The newborns of heavy-marijuana-using mothers had better scores on autonomic stability, quality of alertness, irritability, and self-regulation, and were judged to be more rewarding for caregivers.
This provided reassurance about my patients who used cannabis during pregnancy. Still, I had one more resource to explore.
CHILDREN OF THE COUNTERCULTURE
In the early 1970’s, a group of young adults set out from San Francisco to establish an intentional spiritual community together with the lofty goal of ‘saving the world.’ They bought 1500 acres in Tennessee and began to build a community where they could live in harmony with each other, setting an example for the rest of the world and even reaching out to help others far beyond the boundaries of their own gates. They were young, creating not only a town but also families, delivering their babies at home in the woods of Tennessee. The lay midwives attending the births were exceptionally skilled, guided by a woman named Ina May Gaskin. They named their community The Farm.
This community used cannabis. It was part of their culture and they considered it a sacrament. Except for a brief period of two years, known as the ‘Grass Fast’, almost everyone on The Farm who had access to cannabis smoked it regularly. Women used it while they were pregnant, some during labor, and most during breastfeeding. Here was a population that had exposed their unborn babies to cannabis forty years ago, so it seemed like a good opportunity to check in and see how those babies had fared as they grew up.

In the 4th edition of the book Spiritual Midwifery, there are official statistics on over 1900 Farm births from 1970 to 1994. The incidence of ‘Small for Gestational Age’ or ‘Placental Insufficiency’ was .002% (4 births). Prematurity incidence was .01% (22 births).
I decided to find out how those babies were doing today.
Many of the families eventually left Tennessee to pursue their lofty goals elsewhere, but they are still connected through social media and their collective history as a ‘tribe.’ I contacted the mothers who had been pregnant on The Farm and asked them to take a survey. They were interested and eager to contribute.
I must be clear — this was a survey, not a scientific study. Many of the questions asked for a comment answer, not a check-box answer — so those answers were not statistically easy to report. But after combing through all the data and comments some useful information was revealed.
THE STATISTICS:
LABOR AND DELIVERY
Of surprise interest to me was the use of cannabis during labor and delivery. After all, that is a practice not usually available to women today, but this was a different time and place.The breakdown was right down the middle with 50% finding benefit in cannabis during deliveries. Most comments were positive, but at least one person said that smoking cannabis stalled her labor and only after the effects wore off did she get going again. Yet another indication that this herbal medicine has effects that are very individualistic.
MENTAL ILLNESS AND ADDICTION DISORDERS
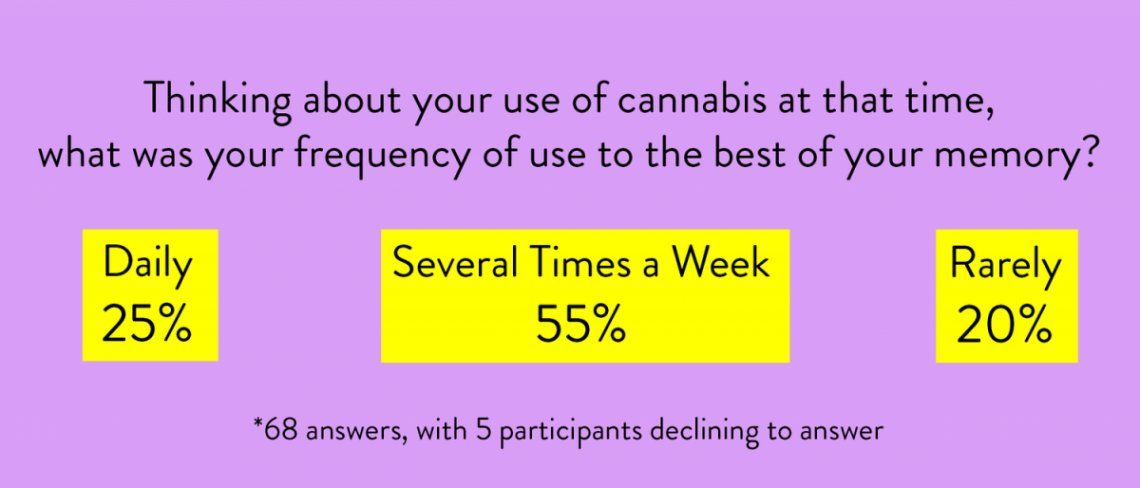
Next, I teased out significant mental illnesses and addiction disorders. 27% of women reported a family history of diagnosed-and-reported bipolar, schizophrenia and suicides. The answers to this section of the survey were important — studies are one thing, but how the children turned out in real life is another. Granted, there were other influences: diet, lifestyle, a self-selected society, questionable memories of family histories, and early use of cannabis by the children — some as young as 7 years old. But taking what the survey gave me, I was able to report the following:


GRASS FAST
I asked questions about the ‘Grass Fast’ (the two years when the entire community abstained) but the answers did not yield any clear results. I had wondered if I could use that time as a ‘control’ since babies gestating during the fast were not exposed, but the information was too vague to provide any clarity.
Comments about the use of cannabis during pregnancy at the end of the survey varied from “I wouldn’t use it now,” to “Cannabis is the greatest, best, most wonderful ally ever and my kids are superstars because of it!” Paraphrased, of course.
WHAT ABOUT THE CHILDREN?
The most impressive part of all this information was showing some of what the children are doing now — are they truly contributing members of society? Are they having difficulty with cognitive thinking? Are they problem citizens?
The following is a list of what these children have grown up to do. I am not ignoring this second generation that did, and do, face problems with mental health and addiction, but I did note that for the most part, those ‘kids’ are doing well. And again, I don’t want to ignore the other factors at play here: diet, personalities that led these individuals to The Farm in the first place, use of other substances, lifestyle and individual family histories.
REPORTED CAREERS, PROFESSIONAL ACCOMPLISHMENTS, AND ACADEMIC ACCOMPLISHMENTSFOR 2ND GENERATION AT THE FARM:
Encouraged, I continued to search for valuable information about the safety of cannabis use while pregnant. Lynn Zimmer, a PhD Associate Professor of Sociology at Queens College in New York, and John P. Morgan, a Professor of Pharmacology at City University Medical School wrote an article for the Drug Policy Alliance in 1997.
They did a complete review of the literature available to them at the time. Their conclusions:
Sixteen years after Dr. Zimmer’s review, this one concluded:
The findings were:
The lower birth weight concern that persists does not seem to be associated with any other problematic factors such as failure to thrive or inability to suckle. As a family physician and a mother, I do consider the fact that any woman who has delivered a baby will agree that if she could get a somewhat smaller baby to push out, one who was perfectly healthy and thrived, she would be grateful for it.
WHAT I TELL MY PATIENTS
After all this reading, reviewing, and surveying, I was left with the following points I could share with my patients:
FOOTNOTES
Revision date:
Aug 29, 2017
CANNABIS USE DURING PREGNANCY: IS IT SAFE?
Dr. Stacey Kerr discusses the controversial topic of cannabis use during pregnancy and gives highlights from her clinical experience with expecting mothers.
Pamela is newly pregnant with her third child. She and her husband think this is going to be their last one because she is having a dreadful time with nausea – morning sickness that lasts all day long. She knows all the tricks. Saltines by her bedside, taking Vitamin B6 and B12, and eating frequently even though her stomach is queasy. She tried ginger. She tried acupuncture. She considered hypnosis. None of it is working, and the added stress of two little ones who still need her attention is making her pregnancy a miserable experience. She really wants this baby, but lately she’s been having guilty doubts about whether it’s worth going through all the nausea and vomiting.
Pamela consulted her physician. She was offered some prescription medications – droperidol (an antipsychotic), metoclopramide (causes drowsiness & dizziness), Benedryl (drowsiness), or Zofran. Although her doctor reassured her about side effects and effects on her baby, she really did not want to take a pharmaceutical if she could avoid it.
Pamela had used cannabis occasionally for many years. It relieved her stress at the end of the day when the kids were finally in bed and she had time to herself. It helped ease some pain she had in the past, and aided sleep when she had short bouts of insomnia. She knew it could help with nausea, appetite, and stress, but she did not know if it was safe to use it while pregnant. So she searched online for facts.
Online, Pamela found conflicting information. Some sites said it was perfectly fine to use cannabis while pregnant. Others warned of brain damage, early labors, babies with failure to thrive, and other dire consequences. There seemed to be some research on the subject, but was it well done? Was it reliable? How was she to dig down and find the real story?
USING CANNABIS WHILE PREGNANT
I am a family physician and have attended hundreds of births during my career. I live in an area of the country (Northern California) where cannabis is used by many of my patients, and when they discovered that they could be honest with me about their use my prenatal records became more complete.
Many mothers use cannabis for nausea and for stress relief.
Many mothers were using it for nausea and for stress relief. Some used it because it was simply part of their lifestyle. We discussed this during their visits, and I was clear with them that I honestly did not know if cannabis caused harm because the scientific research was still incomplete.
In my experience, however, I had not seen complications from cannabis – but I had seen complications from alcohol and other drugs. We discussed the difference between ‘use’ and ‘abuse.’ If they planned to use it I, encouraged conscious use; microdosing to treat the need without overusing.
However, my personal and professional experience was not enough to rely on as a source of information for my patients. I began a search and review of the literature, reading the published peer-reviewed articles, and evaluating the study designs and the outcomes.
FACTS AND RISKS
In this article, we are going to look at the facts. We will look at the research and outcomes, and evaluate their worth. We will look at populations that used cannabis during pregnancy and see how their children are doing now. The information shared may help you make your own decision about using cannabis during pregnancy.
It is important to remember that pregnancy recommendations regarding what to eat, what to drink, what medications to take, and any other outside influences are fraught with caution and fear. If the child does not turn out ‘right,’ who’s fault is it? Pointing a finger of blame can lead to guilt, to lawsuits, and/or a lifetime of regret. Simply being pregnant and carrying a baby for nine months creates unavoidable risks for both mother and baby. But for some, there is no end to the perceived risks or possible harms a mother may cause an unborn child.
Note: The use patterns considered here are limited to well-considered, clearly needed uses of cannabis.This includes using the herb or its constituents for medical reasons such as nausea, pain, sleep, or possibly for stress relief. I encourage any cannabis use to be done consciously, with respect for its power as medicine.
ENDOCANNABINOIDS ARE ESSENTIAL
Before we look at introducing phytocannabinoids to a pregnant mother, let’s consider the endocannabinoid system and the critical role it plays in creating new life. It turns out that our own endocannabinoids, those we create ourselves, are essential to fertilization, growth of the fetus, and survival of a newborn.
- Embryonal implantation into the uterus requires a temporary and localized reduction in one of the most common endocannabinoids present in the brain – anandamide.
- The endocannabinoid system is responsible for neural development by regulating stem cell differentiation into neurons and by guiding axonal migration and synaptogenesis (making the right connections).
- Anandamide protects the developing brain from naturally occurring trauma-induced neuronal loss.
- Suckling initiation in the newborn, which is critical to survival, is stimulated by activation of the CB1receptors in the neonatal brain.
LOW BIRTH WEIGHT, PRETERM LABOR, INCREASED NICU ADMISSIONS?
With the use of cannabis we worry about miswiring the baby’s brain, causing an increase in pregnancy and delivery complications, admissions to the intensive care unit, and problems later in the child’s life such as psychiatric conditions, poor academic achievement, and increased addiction disorders. The possibility of harm caused by using cannabis is a fearful possibility to many pregnant women, their physicians, and midwives.
The most often quoted article in my community was work published in 2011 by Hayatbakhsh and his team, covering a 7-year span of observation in Australia. They interviewed almost 25,000 pregnant women, with over 2400 of these women admitting to ever using cannabis and 637 admitting to use at the time of the interview, during their pregnancy. His conclusions were:
“Use of cannabis during pregnancy strongly and significantly predicted negative birth outcomes, including low birth weight (375 g/.8 lbs lighter), preterm birth, small size for gestational age, and increased admission to the NICU (neonatal intensive care unit).”
Because I had not seen this trend in my own community I read his research carefully. They had controlled for socioeconomic status, multi-substance use, and took into consideration the use of alcohol, cigarettes, and other illicit substances. Their results remained statistically significant.
“Research has suggested that between 8-29% of women use cannabis during pregnancy.”
I kept looking until I found the problem with Hayatbakhsh’s data. First, it was with the method of collection. Pregnant women were interviewed as part of a routine second trimester interview at a public, not private, maternity hospital. Midwives entered the data into a computer, and anyone admitting current use was offered directed care through the hospital’s alcohol and drug specialist service. Any admitted past use was followed by questions on current use.
Now imagine yourself sitting across a desk from a midwife who is providing your care while you are in a vulnerable, pregnant state. She asks you about drug use. Do you tell the truth? Do you admit to something that triggers a referral to a special service for drug abusers? If you answered “yes” to this, you are in the minority. A self-selected group such as this will not lead to the best data, with evidence skewed depending on how many young women were able to be truthful about their use of cannabis.
Surveys done elsewhere support my concern in the data collection process. “Seven percent of pregnant women self-report using marijuana during the prior 2–12 months, although studies measuring marijuana use by self-report or urine screens have identified prevalence ranging from 8% to 29% .”
In addition, there was no long-term follow-up done on any of the mothers or babies from the positive cohort. These weaknesses in the study were enough for me to consider the data questionable. I moved on to the next concern.
ABNORMAL NEURODEVELOPMENT?
Miswiring the brain is a drastic, dramatic, scary thought. No one wants to think they have any avoidable part in harming a baby’s brain. This is a truly serious concern.
A study published in 2011 showed that THC disrupts the natural, highly efficient endocannabinoid signaling in the fetal brain. CB1 receptors in the brain are integral to the development of neural pathways in the developing fetus. The study found that if present, THC will bind to these receptors rather than endocannabinoids.
Researchers dissected brains that tested positive for THC and found those brains to have less of a naturally occurring protein called SCG10, a protein that regulates neuron development. The authors hypothesized that this decrease in SCG10 could cause neurons to develop abnormally both in structure and direction.
Based on an observation, researchers proposed one hypothesis. An alternate hypothesis could be that THCis as efficient as the endocannabinoids. A third hypothesis could be that THC is even more efficient than SCG10. We simply do not know. From this study, all we know is that THC does “promiscuously bind to members of the cannabinoid receptor family.”
Children exposed to marijuana, and not alcohol, in utero were almost 50% better at a behavioral measure of brain processing than controls.
There is an accepted way to measure abnormal neurodevelopment that has been used to evaluate problems like dyslexia, autistic spectrum disorder, and fetal alcohol syndrome. Global Motion Perception (GMP) is a behavioral measure of a type of brain processing that is thought to be particularly vulnerable to abnormal neurodevelopment. GMP is the ability to perceive the whole, rather than focusing only on the individual parts. Imagine watching a football half-time show and being unable to appreciate the pattern the band makes across the field, forced to see only a single tuba player. Those with impaired GMP would only be able to see that tuba player, unable to appreciate the whole picture.
A study published in 2015 measured GMP in 145 4.5-year-old children who had been exposed to different combinations of methamphetamine, alcohol, nicotine, and marijuana prior to birth along with 25 unexposed children. The results were surprising.
As expected, GMP was impaired by prenatal exposure to alcohol. But it was improved significantly by exposure to marijuana! And the direction and size of the effect was unexpected; the children exposed to marijuana in the absence of alcohol were almost 50% better at the GMP task than children with no marijuana exposure. Global motion perception for children exposed to both marijuana and alcohol was no different from that of children who had no drug exposure. Only alcohol and marijuana exposure had independent effects on global motion perception after controlling for the effects of multiple drug exposure, verbal IQ, ethnicity, habitual visual acuity, and sex. Alcohol to the negative, marijuana to the positive.
ACADEMIC ACHIEVEMENT?
The information about neurodevelopment was reassuring, so I moved on to my next concern: academic achievement later in the child’s development. Goldschmidt and his team published research in 2011 that concluded, “First trimester exposure to cannabis significantly predicted poorer academic achievement scores at 14 years of age.”
Here was some long-term follow-up that could be significant.
This research was more difficult to evaluate. It looked like they had accounted for all the possible variables: prenatal alcohol use, tobacco, cigarettes, and other illicit drug exposure. Still, I had not seen this effect of cannabis in my own practice after years of delivering babies and watching those children grow up. What could be the difference?
I called a statistician. After his review, he educated me about ‘mediators.’ Mediators are the factors that must come into play to cause the seen effects. In this case, there were four mediators listed here in order of importance:
- Depression at 10 years old
- An abnormal IQ test at age 6 years
- Inattention noted at age 10 years
- Early use of cannabis before 14 years old
SEVERE MENTAL ILLNESS?
Moving to the next concern, I wondered about the possibility of increased incidence of severe mental illness in children exposed to cannabis during gestation, especially if there was a history of mental illness in the family. This went along with the theory of miswiring brains; if brains were miswired by THC, would this trigger schizophrenia? If teens used cannabis, would they be more likely to develop schizophrenia?
Harvard University and the Boston VA looked at this possibility. The question they set out to answer: “Is family risk for schizophrenia a crucial factor underlying the association between the development of schizophrenia in teens who smoke marijuana?”
They looked at 282 individuals from the New York and Boston metropolitan areas. They gathered information on 1,168 first-degree relatives and a total of 4,291 relatives. They collected information regarding cannabis use, and family history regarding schizophrenia, bipolar disorder, depression, and drug abuse. What they found was that the tendency for depression and bipolar disorder was dependent on family history of these disorders. Their conclusion: “Having an increased familial risk for schizophrenia is the underlying basis for schizophrenia in these samples — not the cannabis use.”
LARGE STUDIES?
Still not completely reassured or satisfied with the available research, I looked for more, and found a study from Carleton University in Ottawa, Canada. Since 1978, psychologist Peter Fried and his colleagues collected longitudinal data on prenatal marijuana exposure as part of the Ottawa Prenatal Prospective Study (OPPS). These researchers administered hundreds of tests to the same group of about 145 children over a 22-year period. The group assessed physical development, psychomotor ability, emotional and psychological adjustment, cognitive functioning, intellectual capacity, and behavior.
At the end of this extensive, long-term study, they found very few differences between marijuana-exposed and nonexposed children. After controlling for known confounding variables, Fried estimated that prenatal drug exposure to alcohol, tobacco, and marijuana combined accounted for 8 percent or less of the variance in children’s scores on developmental and cognitive tests.
Researchers found very few differences between marijuana-exposed and non-exposed children.
Furthermore, no review of this topic would be complete without looking at the work done by Melanie Dreher, a pediatrician who published in the journal Pediatrics in 1994. She looked at children exposed to cannabis in Jamaica. It was a relatively small study – looking at 24 newborns exposed to marijuana prenatally and 20 nonexposed newborns. She found that there were no significant differences between exposed and nonexposed infants on day 3. Then, at 1 month, she found that the exposed infants showed better physiological stability. The newborns of heavy-marijuana-using mothers had better scores on autonomic stability, quality of alertness, irritability, and self-regulation, and were judged to be more rewarding for caregivers.
This provided reassurance about my patients who used cannabis during pregnancy. Still, I had one more resource to explore.
CHILDREN OF THE COUNTERCULTURE
In the early 1970’s, a group of young adults set out from San Francisco to establish an intentional spiritual community together with the lofty goal of ‘saving the world.’ They bought 1500 acres in Tennessee and began to build a community where they could live in harmony with each other, setting an example for the rest of the world and even reaching out to help others far beyond the boundaries of their own gates. They were young, creating not only a town but also families, delivering their babies at home in the woods of Tennessee. The lay midwives attending the births were exceptionally skilled, guided by a woman named Ina May Gaskin. They named their community The Farm.
This community used cannabis. It was part of their culture and they considered it a sacrament. Except for a brief period of two years, known as the ‘Grass Fast’, almost everyone on The Farm who had access to cannabis smoked it regularly. Women used it while they were pregnant, some during labor, and most during breastfeeding. Here was a population that had exposed their unborn babies to cannabis forty years ago, so it seemed like a good opportunity to check in and see how those babies had fared as they grew up.

In the 4th edition of the book Spiritual Midwifery, there are official statistics on over 1900 Farm births from 1970 to 1994. The incidence of ‘Small for Gestational Age’ or ‘Placental Insufficiency’ was .002% (4 births). Prematurity incidence was .01% (22 births).
I decided to find out how those babies were doing today.
Many of the families eventually left Tennessee to pursue their lofty goals elsewhere, but they are still connected through social media and their collective history as a ‘tribe.’ I contacted the mothers who had been pregnant on The Farm and asked them to take a survey. They were interested and eager to contribute.
I must be clear — this was a survey, not a scientific study. Many of the questions asked for a comment answer, not a check-box answer — so those answers were not statistically easy to report. But after combing through all the data and comments some useful information was revealed.
THE STATISTICS:
- 71 responses were included in the report.
- The average age of respondents was 66 years.
- Those 71 women reported on a total of 178 children who were born while living at The Farm.
- The average length of time lived at The Farm culture was 12 years.
- The second generation birth years spanned from 1971 to 1991. This is significant in that it represents a time when cannabis generally had a lower THC content than it is today.
- 54% of the children were male, 46% were female with a ratio of 1.20. This is slightly higher shifted towards boys compared to the USA average of ~1.07.
- 11% of the women reporting did not use cannabis, and 89% did use cannabis.
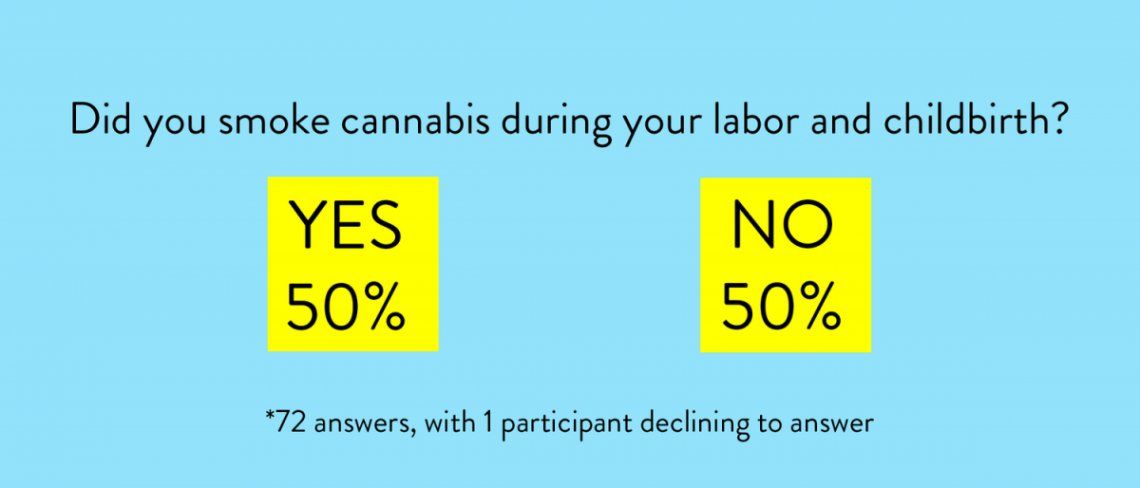
LABOR AND DELIVERY
Of surprise interest to me was the use of cannabis during labor and delivery. After all, that is a practice not usually available to women today, but this was a different time and place.The breakdown was right down the middle with 50% finding benefit in cannabis during deliveries. Most comments were positive, but at least one person said that smoking cannabis stalled her labor and only after the effects wore off did she get going again. Yet another indication that this herbal medicine has effects that are very individualistic.
MENTAL ILLNESS AND ADDICTION DISORDERS
Next, I teased out significant mental illnesses and addiction disorders. 27% of women reported a family history of diagnosed-and-reported bipolar, schizophrenia and suicides. The answers to this section of the survey were important — studies are one thing, but how the children turned out in real life is another. Granted, there were other influences: diet, lifestyle, a self-selected society, questionable memories of family histories, and early use of cannabis by the children — some as young as 7 years old. But taking what the survey gave me, I was able to report the following:
GRASS FAST
I asked questions about the ‘Grass Fast’ (the two years when the entire community abstained) but the answers did not yield any clear results. I had wondered if I could use that time as a ‘control’ since babies gestating during the fast were not exposed, but the information was too vague to provide any clarity.
Comments about the use of cannabis during pregnancy at the end of the survey varied from “I wouldn’t use it now,” to “Cannabis is the greatest, best, most wonderful ally ever and my kids are superstars because of it!” Paraphrased, of course.
WHAT ABOUT THE CHILDREN?
The most impressive part of all this information was showing some of what the children are doing now — are they truly contributing members of society? Are they having difficulty with cognitive thinking? Are they problem citizens?
The following is a list of what these children have grown up to do. I am not ignoring this second generation that did, and do, face problems with mental health and addiction, but I did note that for the most part, those ‘kids’ are doing well. And again, I don’t want to ignore the other factors at play here: diet, personalities that led these individuals to The Farm in the first place, use of other substances, lifestyle and individual family histories.
REPORTED CAREERS, PROFESSIONAL ACCOMPLISHMENTS, AND ACADEMIC ACCOMPLISHMENTSFOR 2ND GENERATION AT THE FARM:
- Nurse (several)
- Nurse Practitioner–Women’s Health and MS
- Occupational Therapist
- Painting Contractor
- Peace Corps–dual Masters in Sustainable Development and International Relations
- Photojournalist
- Physician (MD)
- Professional Actor
- Professional MMA fighter–Ranked in the top 10 for the last 11 years
- Project Manager for large IT corporation
- Second City Improv Performer
- Senior Level Iyengar Yoga Instructor
- Silicon Valley Tech Executive
- Software Engineer/System Administrator
- Software Designer
- Teachers–Kindergarten, ESL, International, Bilingual, etc.
- Web Developer
- Woodworking Craftsman
- Aquatic Biologist
- Artist (several)
- Attorney (several)
- Banking VP–Financial Analyst
- Biotech Executive
- Carpenter
- Civil Engineer for Army Corps of Engineers
- Contractor
- Electronic Navigation Device Development for DOD
- Ergonomist
- Homicide Investigator for the DA, speaks 7 languages and works with police and gangs
- IT Reverse 911 mapping for France
- Master Plumber
- Masters Degree in Classical Language
- Masters Degree
- Mechanic and Angora Goat Farmer
- Midwife
- Motivational Speaker
- Musician (several)
Encouraged, I continued to search for valuable information about the safety of cannabis use while pregnant. Lynn Zimmer, a PhD Associate Professor of Sociology at Queens College in New York, and John P. Morgan, a Professor of Pharmacology at City University Medical School wrote an article for the Drug Policy Alliance in 1997.
They did a complete review of the literature available to them at the time. Their conclusions:
- Adverse outcomes are inconsistent from one study to another.
- Marijuana contributes less than alcohol or tobacco.
- The findings show no consistent relationship of fetal harm to either the timing or degree of marijuana exposure.
- The weight of current scientific evidence suggests that marijuana does not directly harm the human fetus.
Sixteen years after Dr. Zimmer’s review, this one concluded:
- There may be some effects noted in older children.
- If these effects do exist with light, moderate, or sporadic use, they are sufficiently subtle as to not be consistently demonstrated between studies.
- Based on these findings, mandatory reporting of marijuana use during pregnancy and punitive measures related to the use of this drug during pregnancy or breast-feeding do not seem medically warranted.
The findings were:
- Increased anemia in mothers.
- Decreased birth weight, increased NICU admissions.
- Tobacco & alcohol included in too many studies.
- Relied on self-reported use of cannabis.
- Studies with conflicting results so definitive conclusions not drawn.
- Bottom line: More research needs to be done.
The lower birth weight concern that persists does not seem to be associated with any other problematic factors such as failure to thrive or inability to suckle. As a family physician and a mother, I do consider the fact that any woman who has delivered a baby will agree that if she could get a somewhat smaller baby to push out, one who was perfectly healthy and thrived, she would be grateful for it.
WHAT I TELL MY PATIENTS
After all this reading, reviewing, and surveying, I was left with the following points I could share with my patients:
- Cannabis can be abused. Don’t abuse it.
- Smoke is an irritant on the airways. If you wish to inhale, vaporize flowers or use an alternate form of the medicine.
- Federal law prohibits cannabis
- Hospitals, physicians, and Social Services can have punitive responses to parents who test positive for THC.
- Babies exposed to cannabis during gestation may weigh less than babies not exposed.
- Be clear about why you are using it and re-evaluate those reasons each time
- Avoid smoking – vaporize herb or use non-smoked products from trusted sources
- Use organic herb and concentrates that are clear of chemicals and pesticides
- Be aware of the cannabinoid content and microdose medicine to efficacy
- Keep your children safe from accidental or passive exposure
- Avoid dabs, oils, and edibles with unknown content
FOOTNOTES
- E Fride, Multiple Roles for the Endocannabinoid System During the Earliest Stages of Life: Pre- and Postnatal Development, J Neuroendocrinol. 2008 May;20 Suppl 1:75-81. doi: 10.1111/j.1365-2826.2008.01670.x
- R. Hayatbakhsh, etal, Birth outcomes associated with cannabis use before and during pregnancy, Mohammad Pediatr Res 71: 215-219, December 21, 2011; doi:10.1038/pr.2011.2
- Ko JY, Farr SL, Tong VT, Creanga AA, Callaghan WM. Prevalence and Patterns of Marijuana Use among Pregnant and Non-Pregnant Women of Reproductive Age. Am J Obstet Gynecol. 2015
- Chang J, Holland C, Tarr J, Rodriguez K, Kraemer K, Rubio D, Arnold R. Direct observation of screening for and disclosure of illicit drug use in pregnancy visits. American Journal of Health Promotion. 2015 In Press
- E. Keimpema, Molecular model of cannabis sensitivity in developing neuronal circuits, Trends Pharmacol Sci. 2011 Sep;32(9):551-61. doi: 10.1016/j.tips.2011.05.004.
- Arijit Chakraborty, etal. Prenatal exposure to recreational drugs affects global motion perception in preschool children. Scientific Reports, 2015; 5: 16921 DOI: 10.1038/srep16921
- Goldschmidt L, et al, School achievement in 14-year-old youths prenatally exposed to marijuana, Neurotoxicol Teratol,(2011), doi:10.1016/j.ntt.2011.08.009
- AC Proal, et al, A controlled family study of cannabis users with and without psychosis, Schizophrenia Research, Volume 152, Issue 1, January 2014, Pages 283–288 doi:10.1016/j.schres.2013.11.014
- Fried, P.A., Prenatal exposure to tobacco and marijuana: effects during pregnancy, infancy, and early childhood. Clinical Obstetrics and Gynecology 36:319-337, 1993.
- Melanie C. Dreher, etal, Prenatal Marijuana Exposure and Neonatal Outcomes in Jamaica: An Ethnographic Study, Pediatrics, Feb 1994, 93 (2) 254-260
- Spiritual Midwifery Third Edition, Ina May Gaskin, The Book Publishing Company, Summertown, TN
- Use of Marijuana during Pregnancy, Article excerpted from Marijuana Myths, Marijuana Facts: A Review of the Scientific Evidence by Lynn Zimmer, PhD, and John P. Morgan, MD (New York: Drug Policy Alliance, 1997)
- Meg Hill, MBBS, and Kathryn Reed, MD, Pregnancy, Breast-feeding, and Marijuana: A Review Article, CME Review Article, Volume 68, Number 10, Obstetrical and Gynecological Survey, Copyright 2013
- Gunn JKL, Rosales CB, Center KE, et al., Prenatal exposure to cannabis and maternal and child health outcomes: a systematic review and meta-analysis. BMJ Open 2016;6:e009986. doi:10.1136/bmjopen-2015-009986
- Health Effects of Cannabis and Cannabinoids - The Current State of Evidence and Recommendations for Research, published by the National Academies of Sciences, 2017
Revision date:
Aug 29, 2017